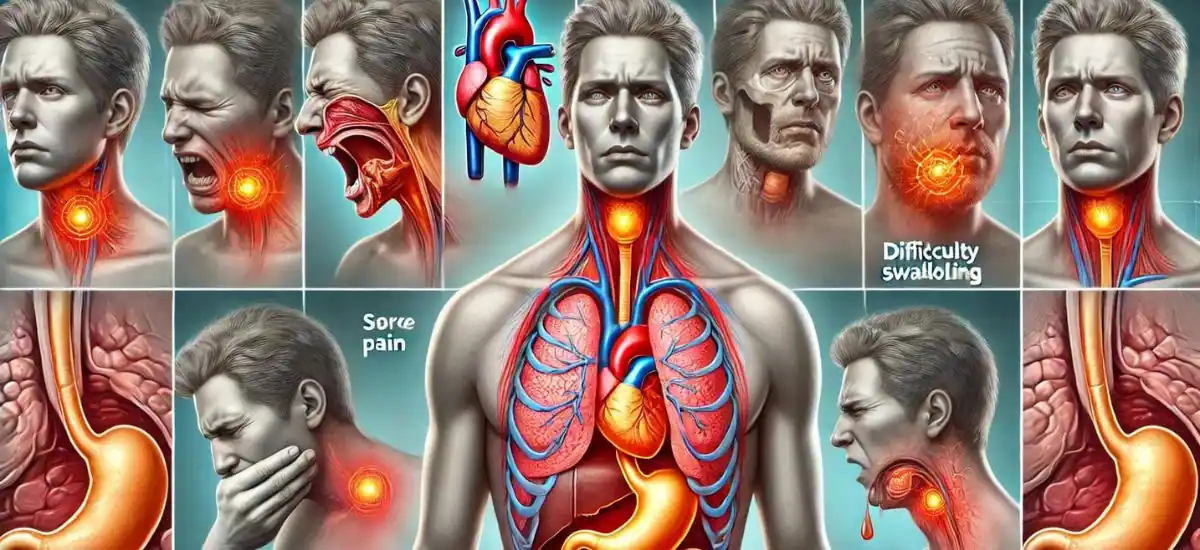
Gastroesophageal Reflux Disease (GERD) is a chronic condition where stomach acid frequently flows back into the tube connecting your mouth and stomach (esophagus). This acid reflux can irritate the lining of your esophagus, leading to GERD. The most common symptoms of GERD include heartburn—a burning sensation in the chest that often occurs after eating and might be worse at night—and regurgitation of food or sour liquid.
Other symptoms might include difficulty swallowing, chronic cough, a sensation of a lump in the throat, and disrupted sleep. Recognizing these symptoms is crucial for effective management and preventing complications such as esophageal damage. Early diagnosis and treatment can significantly improve the quality of life for those affected by GERD.
Common Symptoms of GERD

- Heartburn: Often described as a burning sensation that starts in the stomach and annoyingly works its way up to the chest and even the throat. It’s like a fire within that can flare up, especially after a big meal or during the night.
- Regurgitation: This isn’t your average upset stomach. Imagine tasting your lunch for the second time, but not by choice. It’s acidic, it’s bitter, and it can leave a nasty taste in your mouth.
- Dysphagia: Sometimes, swallowing can feel like a challenge. Food seems to linger in the throat or chest, creating an uncomfortable sensation of blockage. It’s not just aggravating; it can be downright alarming.
Less Common Symptoms That May Indicate GERD
GERD can be quite the crafty condition, presenting symptoms that many might not immediately associate with acid reflux:
- Chest Pain: This can be a sharp, burning pain that might make you think you’re having a heart attack. But before you panic, consider that GERD is often the culprit behind such scares.
- Hoarseness or Sore Throat: Frequent acid reflux can irritate your throat and vocal cords, leading to a hoarse voice or a persistent sore throat that doesn’t seem to go away with the usual remedies.
- Persistent Cough: A cough that lingers, particularly after meals or at night, can be a subtle sign of GERD. It’s the kind of cough that makes you wonder why it’s sticking around so long.
Symptoms of GERD in Different Populations
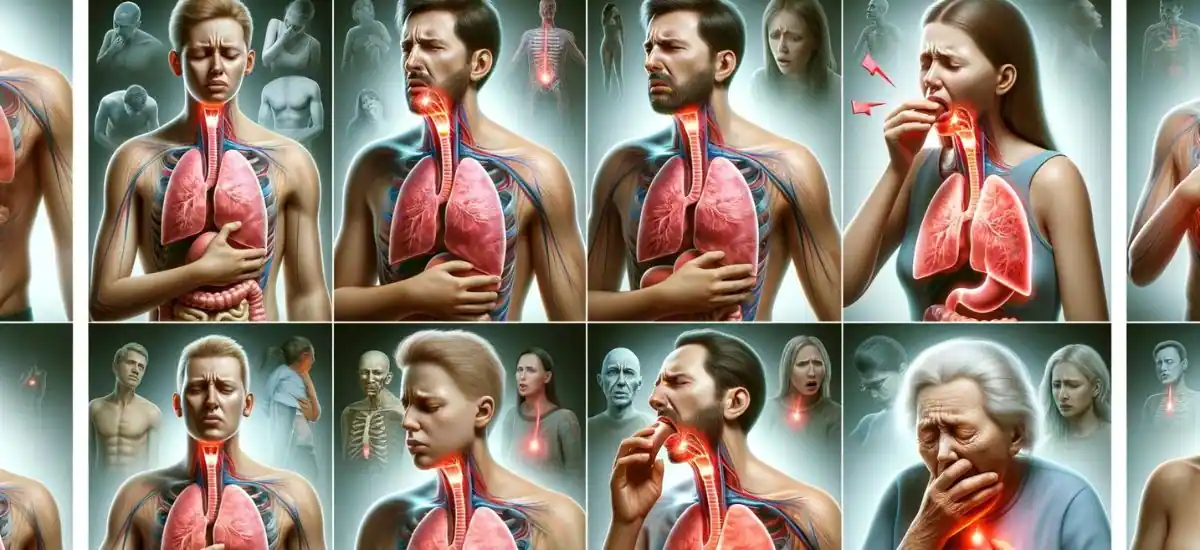
GERD doesn’t play favorites—it can affect anyone, but symptoms might look different across various age groups:
- Infants and Children: It’s tough when the little ones can’t tell us what’s wrong. Look for signs like spitting up more than usual, irritability during feeding, or refusal to eat. These could be clues that your child is experiencing GERD.
- Elderly: As we age, our bodies don’t always cooperate like they used to. Older adults might experience less obvious symptoms, such as increased salivation, or finding it hard to swallow their food. It’s not just a part of getting older—GERD could be to blame.
When to Seek Medical Help
Navigating when to reach out for medical assistance can be a lifesaver, especially when dealing with GERD’s more severe or persistent symptoms:
- Troublesome Symptoms: Don’t brush off severe chest pain, difficulty swallowing, or persistent vomiting as just another bad day. These symptoms can indicate a serious progression of GERD or other medical emergencies. It’s critical to contact your healthcare provider immediately to rule out more severe conditions like a heart attack or a blockage.
- Symptoms Persisting: GERD can be stubborn. If your throat is often on fire and over-the-counter antacids are as effective as a band-aid on a broken leg, it’s time to escalate the issue. Chronic symptoms that resist basic treatment efforts warrant a closer look by a professional. Consistent or worsening symptoms can lead to complications like esophagitis or even esophageal cancer. Regular medical consultations can prevent these potentially severe outcomes and help manage your condition more effectively.
Diagnosis of GERD
Diagnosing GERD is a thorough process that involves several steps to ensure an accurate assessment and appropriate treatment plan:
- Diagnostic Tests: Medical technology comes to the rescue with tools like upper endoscopy and esophageal pH monitoring, which are more than just medical jargon. An endoscopy allows doctors to look directly inside your esophagus and stomach to check for inflammation or damage caused by stomach acid. Meanwhile, pH monitoring measures acid levels in your esophagus for 24 to 48 hours to see how often and how long acid regurgitation occurs. These tests are crucial in confirming GERD and understanding the severity of your condition.
- Discussing Your History: This isn’t just small talk; it’s a deep dive into what you’ve been experiencing. Your doctor will need detailed information about your symptoms: their frequency, triggers, and what you’ve done to try to alleviate them. This comprehensive discussion is vital to develop an effective treatment strategy tailored to your specific needs and lifestyle. It’s your opportunity to be heard and to take an active role in managing your health.
Frequently Asked Questions
Q1. What lifestyle changes can help manage GERD symptoms?
Ans: To manage GERD, try eating smaller meals, avoiding trigger foods like spicy dishes and caffeine, staying upright after meals, and losing excess weight. Elevating the head of your bed and quitting smoking can also be beneficial.
Q2. Can GERD symptoms be treated with over-the-counter medications?
Ans: Yes, over-the-counter antacids and H2-receptor blockers can provide relief by neutralizing stomach acid or reducing acid production. However, consult a doctor if symptoms persist.
Q3. Is GERD a permanent condition?
Ans: GERD can be a chronic condition, but many people manage it effectively with lifestyle changes and medication. In some cases, surgical options might be considered if conventional treatments are ineffective.
Conclusion
Rounding off, we’ve covered the primary symptoms of GERD and explored how they can differ among various age groups. We’ve also touched on when it’s wise to seek medical advice and what to expect during diagnosis. If you’ve been nodding along thinking, “That sounds like me,” it might be time to chat with your healthcare provider. GERD is manageable, especially with early detection and the right approach.